Curated from the article "Patient Positioning During Thoracentesis Solved" on February 4, 2020 by Safe Patient Handling Medical. Read the original article here.
Patient Handling Hazards
Rates of musculoskeletal injuries from overexertion in healthcare occupations are among the highest of all U.S. industries. Data from the Bureau of Labor Statistics (BLS) show that in 2014, the rate of overexertion injuries averaged across all industries was 33 per 10,000 full time workers. By comparison, the overexertion injury rate for hospital workers was twice the average (68 per 10,000), the rate for nursing home workers was over three times the average (107 per 10,000), and the rate for ambulance workers was over five times the average (174 per 10,000).1
The single greatest risk factor for overexertion injuries in healthcare workers is the manual lifting, moving and repositioning of patients, residents or clients, i.e., manual patient handling.
Safe Patient Handling
Over the past two decades major advancements have occurred in patient care including many new safe patient handling solutions developed to help our nurses and caregivers avoid the risk of injury. Manual patient handling is one of the leading causes of back injuries for nurses. As a result, many states have enacted laws to mandate that hospitals follow a Safe Patient Handling program. Required programs evaluate all inpatient units for high risk tasks that involve lifting, pushing, pulling, or prolonged static holds and evaluating solutions to lessen the risk(s).
Risky Positioning
One example of a common inpatient procedure that puts the ultrasound/imaging team, patient and nursing staff at risk for injury is Thoracentesis. According to the National Heart, Lung, and Blood Institute, “Thoracentesis is a procedure in which a needle is inserted into the pleural space between the lungs and chest wall. This procedure is done to remove excess fluid, known as a pleural effusion, from the pleural space to help patients breathe easier.”
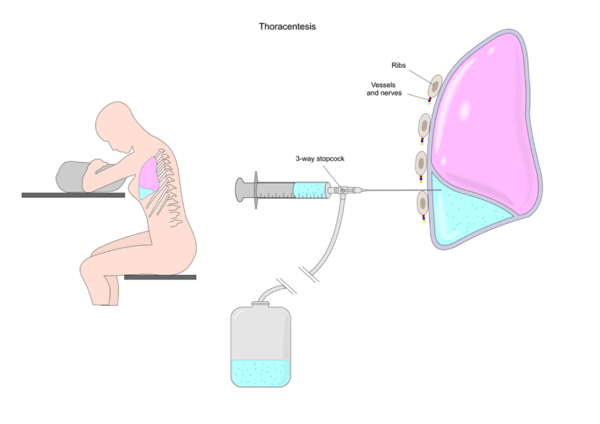
Image via Shutterstock |
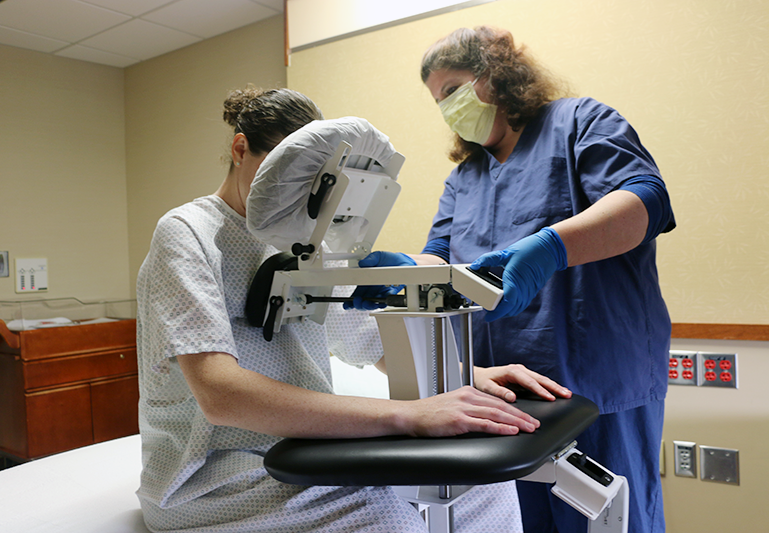
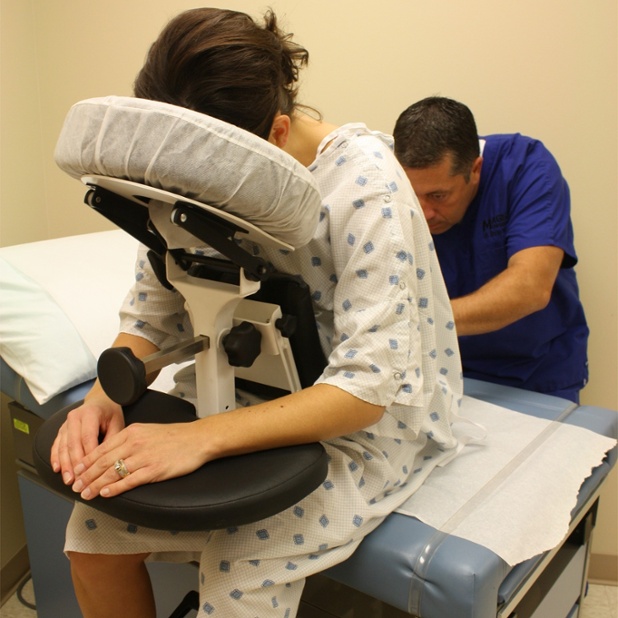
Thoracentesis is performed in a doctor’s office or hospital. The procedure usually takes 10 to 15 minutes, unless a patient has a large amount of fluid in the pleural space. For the procedure, most patients sit quietly on the edge of a chair or bed with their head and arms resting on a table. A nurse or LPN usually assists the patient to get into position by maneuvering a bedside tray table and utilizing a stool to support the patient’s feet. Pillows may be stacked on the table for the patient to lean on comfortably. Unfortunately, most bedside tables do not lock securely into place and the table can become an unstable tipping hazard. Risky positioning such as using unsteady tables with pillows does not benefit the patient or medical staff, and can lead to unnecessary risk and injury.

Photo 1: Unstable bedside table, stool and pillow |

|
Ultrasound may be used to determine the best location to insert the needle. After cleaning the skin around the area where the needle will be inserted, the doctor will inject a local anesthetic to numb the area. A needle is inserted between the ribs into the pleural space. There may be a sensation of discomfort or pressure when the needle is inserted. As the doctor draws out excess fluid from around the lungs, there may be a feeling like coughing or chest pain. The needle will be removed, and a small bandage will be applied to the site.
Preventing Injury with Safe Patient Positioning
Proper positioning is critical for patient safety. Evidence-based research has shown that safe patient handling solutions can significantly reduce overexertion injuries by replacing manual patient handling with safer methods guided by the principles of “Ergonomics.”² Ergonomics refers to the creation of tasks best suited to the capabilities of workers. In the case of patient handling, it involves the use of mechanical equipment and safety procedures to lift and move patients so health care workers can avoid using manual exertions thereby reducing their risk of injury. In addition, patient handling ergonomics seeks to maximize the safety and comfort of patients during handling.
Using the Epidural Positioning Device
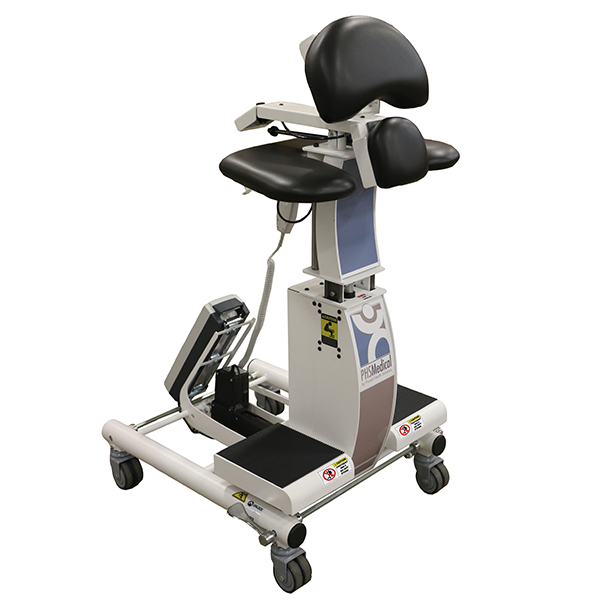
The Epidural Positioning Device is the key to solving risk factors associated with administering Thoracentesis and all manual patient handling situations such as static holds and fall risks. Designed by an anesthesiologist, the Epidural Positioning Device helps position patients correctly and comfortably by encouraging cervical, thoracic and lumbar flexion while maintaining a solid and stable position. Manually controlled chest, arm and head support ensures that patients of every body type and size can be accommodated, and the spine remains immobile during epidural placement. The EPD is suitable for use in operating rooms, labor and delivery suites, pain centers or anywhere epidural and spinals are performed. The EPD stand provides adjustable foot support to aid in positioning the patient and for patient comfort. It also provides an adjustable mount for the EPD and features a built-in clamp allowing for the same range of adjustment as an operating room table.
  |
|
Sources:
1 Bureau of Labor Statistics Table R8. Incidence rates for nonfatal occupational injuries and illnesses involving days away from work per 10,000 full-time workers by industry and selected events or exposures leading to injury or illness, private industry, 2014pdf iconexternal icon.
2 Waters, T., Putz-Anderson, V., Fine, L. [1993]. Revised NIOSH equation for the design and evaluation of manual lifting tasks. Ergonomics, 36, 749-776. Please Note: A Special Section entitled “Impact of Thomas Waters on the Field of Ergonomics,” has been published in Human Factors: The Journal of the Human Factors and Ergonomics Society, August 2016 58:665-795. View the Preface to the Special Sectionpdf iconexternal icon
3 Centers For Disease Control and Prevention
https://www.cdc.gov/niosh/topics/safepatient/default.html#Patient%20Handling%20Ergonomics