This blog was curated from a podcast posted on May 2, 2018 by Dr. Roger Browning. Listen here.
Super morbid obesity is defined as a having a Body Mass Index >50. The physiological and anatomical changes associated with the super morbidly obese population introduce a number of unique considerations for anesthesia management. From monitoring blood pressure, to inserting an IV, or administering an epidural, obese and overweight patients can be harder to safely move, leading to inefficiencies and stress on both the patient and medical staff. Here are some practical tips on how to navigate the challenges they can present.
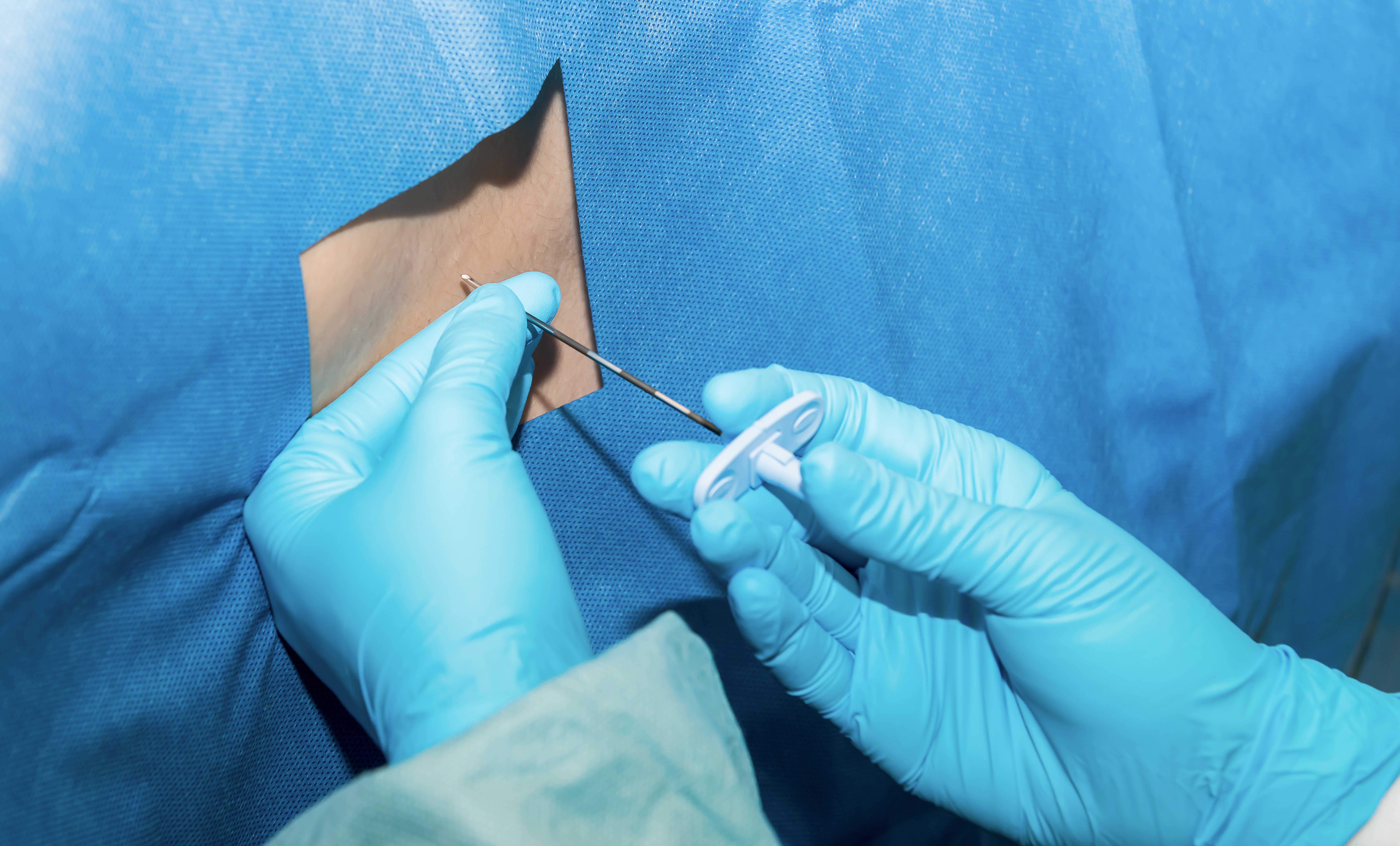
Epidural injection image via Shutterstock |
Practical Tips and Hints
- Blood pressure monitoring. Using cuffs on the upper arm often does not work well. Instead, consider a standard adult cuff placed on the forearm or if in theatre, put in an arterial line.

Image via Shutterstock
- Use ultrasound to get reliable intravenous access. Administer two IVs if in theatre as they tissue easily, and you will want to have a spare in case one stops working halfway through surgery.
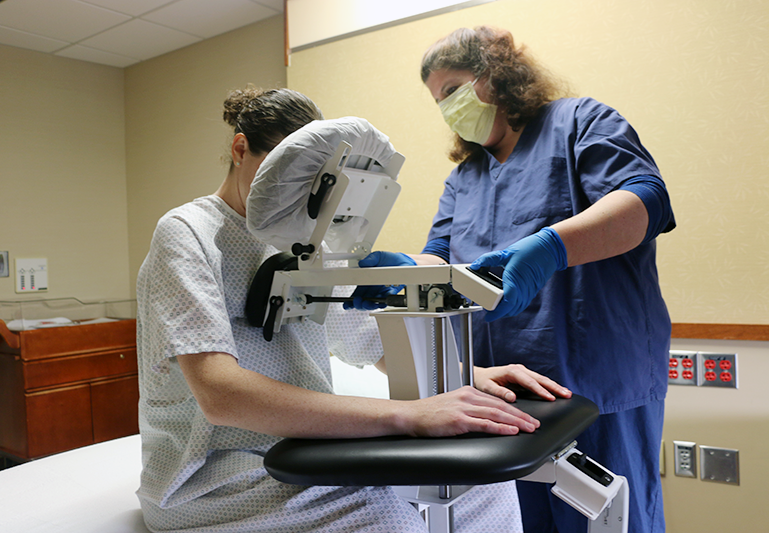
- Use caution with manual handling and positioning issues. Employ correct patient positioning with epidural positioning devices (not people, chairs, pillows or stools). Also, use enough staff to carefully and safely move the patient.
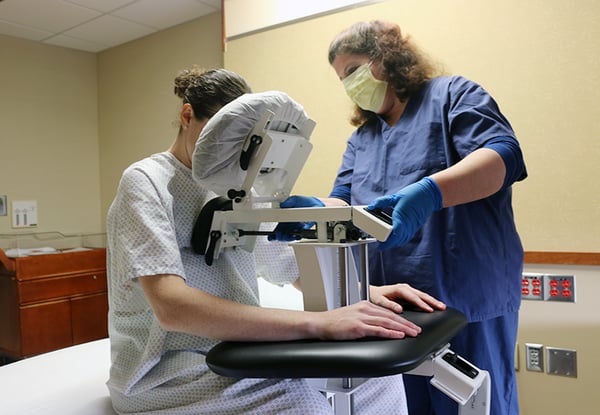
Epidural Positioning Device via PHS Medical |
4. Utilize ultrasound when attempting a neuraxial block. Ultrasound-assisted neuraxial block is an advanced technique for use in patients with difficult spinal anatomy. The practice of central neuraxial block (CNB) has traditionally relied on the palpation of bony anatomical landmarks, namely the iliac crests and spinous processes, together with tactile feedback during needle insertion. However, these landmarks may be difficult to identify accurately—a problem exacerbated by altered patient anatomy, including obesity, age-related changes, and previous spinal surgery. The use of a pre-procedural scan improves the technical efficiency of central neuraxial block (CNB) by facilitating precise identification of underlying anatomical structures.³
5. Keep extra-long Tuohy and spinal needles nearby. The distance to the epidural space is greater in patients with an increased body mass index. Therefore, longer than standard spinal and epidural needles including Tuohy needles may be needed and should be readily available.

image via Shutterstock |
6. Anticipate potential obstructive sleep apnea & respiratory issues and be very careful with opioids and sedatives. Use non-sedating regional analgesia/NSAIDs.
References
1. Tunnelling Epidural Catheters: An editorial discussing tunnelling of epidural catheters to prevent accidental catheter migration and Dr Pavy’s famous 1994 article.
- Tunnelling epidural catheters: a worthwhile exercise? Editorial N. Kumar W. A. Chambers
- Anaesth Intensive Care. 1994 Dec; 22(6):703-5. Tunnelled epidural catheters for routine use: description of a technique. Pavy TJ1.
2. Management of super morbidly obese parturient with two epidural technique:
3. Utilizing ultrasound with a neuraxial block:
https://academic.oup.com/bjaed/article/16/7/213/2196372